CT VS. MRI
When a patient with suspected neurological disease presents to Veterinary Neurology & Imaging of the Chesapeake, there are a number of steps in the process of identifying, diagnosing and treating their condition. The first step includes a thorough physical and neurologic exam to evaluate the patient’s symptoms and neurologic capabilities. From the examination, we assess the location of the problem and create a rule-out list. From this, we will perform confirmatory advanced neurodiagnostics such as magnetic resonance imaging (MRI) or computed tomography (CT). Both CT and MRI use powerful computers to reconstruct the anatomy in three dimensions.
There are a number of factors to consider when selecting CT versus MRI for a given neurologic case. As with any diagnostic test, the neurologist has to consider the most likely differential diagnoses in consideration with the accuracy of the imaging for those specific differentials. Those factors must be weighed against the risks and benefits of the test.
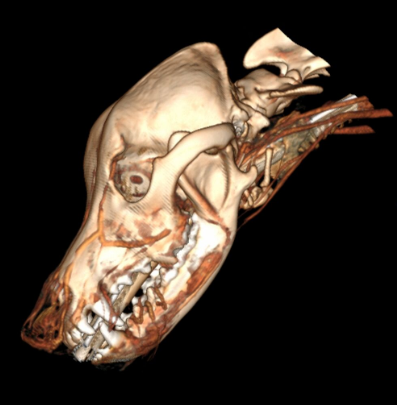
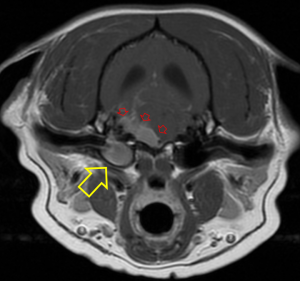
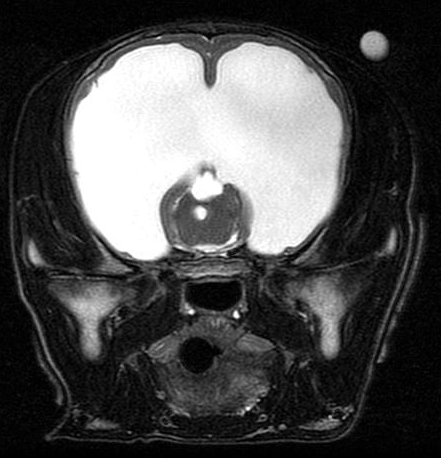
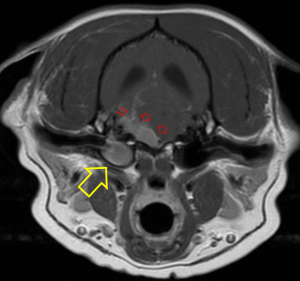
When considering which imaging modality is ideal, it can be challenging to give a simple uniform answer but, in general, MRI is superior for resolution of soft tissue lesions. MRI uses powerful magnetic fields and radio frequency pulses to produce detailed pictures of organs, soft tissues, bone and other internal body structures. CT uses radiation (X-rays – just like radiographs) so it is best for discriminating tissues with different densities, such as bone, air and water (tissue).
MRI tends to cost more, is less widely available and acquisition can take longer. Anesthesia is practically required for MRI, while CT due to its rapid acquisition, can be done with heavy sedation or in some cases, simple restraint.
With that said, in cases where a brain lesion is suspected, MRI is more sensitive and specific in almost every patient to diagnose primary or metastatic brain tumors, encephalitis, vascular lesions and degenerative disorders. For spine lesions, MRI is better for disc extrusions, soft tissue tumors (e.g. meningioma) and intraparenchymal lesions (FCE, meningomyelitis, syringomyelia).
The power of CT is the use in acute head trauma, spinal fractures, bony neoplaisia, some nasal tumors and otitis media/externa. CT is often used in emergency cases due to availability and its short scan time.
In a case where MRI may be primarily indicated but an owner elects to proceed with CT due to cost or risk, it is important to note that the results can be non-specific and the patient may require MRI if the CT results come back inconclusive or normal.
A Comparison of CT vs. MRI
|
|
CT | MRI |
| Radiation exposure | The effective radiation dose from CT ranges from 2 to 10 mSv, which is about the same as the average person receives from background radiation in 3 to 5 years. | None. MRI machines do not emit ionizing radiation. |
| Time required to complete scan | Typically 10-20 minutes – some studies can be done under sedation | Typically 40-60 minutes – due to the loud noises during the study, anesthesia is required |
| Effects on the body | CT can pose the risk of irradiation. Painless, noninvasive. | No biological hazards have been reported with the use of MRI. |
| Application | Suited for bone injuries, lung and chest imaging, cancer detection. Widely used on Emergency Room patients. | Suited for soft tissue evaluation- spinal cord injury, brain, ligament and tendon injury |